On July 4, 2025, President Trump signed into law H.R. 1, or the “Big Beautiful Bill,” which the Congressional Budget Office predicts will cut Medicaid spending by nearly $1 trillion over the next decade. Due to these changes, many San Franciscans will lose insurance coverage from Medi-Cal, California’s Medicaid, falling back instead on the city’s own healthcare program, Healthy San Francisco (HSF).
Additionally, three weeks ago, due to Congress’s failure to pass a federal funding bill, the government shut down. A funding extension proposed by the Republican majority was blocked by the Democratic Party in an attempt to use the shutdown as political leverage in a fight over healthcare. One of Democrats’ central demands is the reversal of the Medicaid cuts passed this summer.
Deena Lahn is the Vice President of Policy and External Affairs at the San Francisco Community Clinic Consortium (SFCCC), a network of twelve safety-net community health centers in the city. The term “safety-net” refers to an organization that serves people regardless of their insurance status or ability to pay.
Lahn explained that public healthcare coverage has generally increased in her twelve years at SFCCC, but these drastic Medicaid cuts reversed that trend. “My whole career has been…I’m not saying every day was happy, but basically all progress, progress, progress,” she said. “My job has gotten to be a lot less fun in the last six months. Now, a lot of times I’m giving bad news instead of good news to my clinics.”
How H.R. 1 Restricts Medi-Cal Access
On January 1, 2026, Medi-Cal will no longer accept new enrollments from people with unsatisfactory immigration status (UIS), a term that includes undocumented immigrants as well as recent green card recipients, those with refugee status and those seeking asylum. Children, pregnant women and anyone already enrolled in Medi-Cal will remain covered. However, by July 1, 2026, all adults with UIS will stop receiving dental insurance.
Although the SFCCC is working to frontload Medi-Cal enrollment before 2026, they have met obstacles, Lahn said. “We’re already seeing some people who don’t want to sign up for Medi-Cal…I think it’s kind of scared a lot of people.”
On January 1, 2027, California will implement an H.R. 1-mandated work requirement of 80 hours a month, which Governor Gavin Newsom predicts will prevent over three million Californians from accessing Medi-Cal, largely due to administrative barriers. “Other states’ experiences demonstrate that work requirements do not increase employment among enrollees,” according to a Labor Center report by the University of California, Berkeley. “Instead, their onerous documentation requirements increase administrative costs and reduce enrollment and access to care.”
Olivia Burke, a health policy consultant at Faulkner Consulting Group, says the term “work reporting requirement” would be more accurate, pointing out that the change creates barriers specifically for people with fewer resources.
“You’re thinking about a low-income population who doesn’t necessarily have the same access, right?” she said. “Is it actually paper documents that you have to submit to an office? Are you able to access it on a phone? Do you have phone service?… reporting requirements can make it really difficult for people to get coverage, even if they are working,” Burke said.
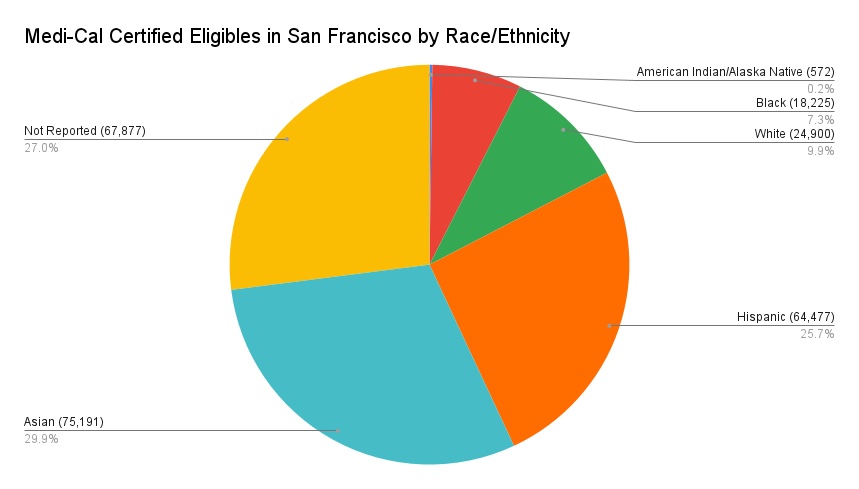
Data as of August 14, 2025 from the State of California, Department of Health Care Services, Medi-Cal Certified Eligibles, by County and Dual Status
The City’s Fallback Program: Healthy San Francisco
These are drastic changes. However, San Francisco is resilient. The San Francisco Department of Public Health (DPH) has, since 2007, run a city-wide healthcare program called Healthy San Francisco (HSF).
HSF was the city’s plan to provide universal healthcare and remains the city’s fallback healthcare program for all San Francisco residents. It is accepted in place of insurance at the Zuckerberg San Francisco General Hospital (SFGH) and clinics such as the SFCCC throughout the city.
Notably, HSF is limited—the program does not extend outside of the city, and does not cover vision or dental care. Because of these constraints, it does not qualify as insurance. Certain procedures—like a bone density scan, which SFGH typically outsources to UCSF—would not be available to someone on HSF.
HSF is largely funded by the city, along with either employer fees or individual payments based on a sliding scale. At its peak, HSF covered nearly 40,000 people—but as Medi-Cal grew its coverage, the need for HSF decreased. By 2024, only 6,000 people were enrolled.
However, Lahn noted, with the expected impact of H.R. 1, that number is expected to grow rapidly. “We’re working together with the city and county of San Francisco to try to figure out, now that more people are again going to come on Healthy San Francisco, how are we going to manage this?” she said.
H.R. I’s Impact on San Francisco’s Healthcare System
Originally, Medi-Cal and similar public health insurance programs were much more restricted than they are today. Though these H.R. 1 cuts were primarily to extend Trump’s tax cuts, Lahn explained that they were also ideologically and financially motivated. The federal government spent nearly $600 billion on Medicaid in 2024. “Their point of view is that the Medi-Cal program was designed a certain way, and that we’ve expanded too much,” she said.
Mary Lawrence Hicks, a nurse practitioner at an SFCCC clinic, the San Francisco Community Health Center in the Tenderloin, expressed a differing view.
“Keeping people healthy is less expensive, ultimately, to the system…if somebody develops a catastrophic illness, they go into the emergency room. They need to be admitted for whatever this thing is. They need to go to the ICU. All of that the hospital has to cover…it’s illegal not to treat them. So if they’re not getting their basic primary care…they’re more at risk for catastrophic illness, and then they’re gonna cost the system more,” she said. “It’s not a smart way to run things. It’s not compassionate, but it’s also not even smart.”
Burke further emphasized the importance of care. “The human cost is really high. When you think about people who lose access to coverage and are no longer able to see their doctors or to fill prescriptions…the sense of precarity that can create in someone’s life…we know that people, when they don’t have insurance, delay or forego care, and that can have real and severe impacts on people’s health,” she said.
Additionally, as H.R. 1 regulations come into effect, fewer patients will be insured, and more of the financial burden will fall on healthcare providers. Lahn voiced uncertainty about the shifting landscape. “I know that the clinics are really committed to continuing to serve everybody, but eventually something will have to change, with this much less money in the system,” she said.
Dr. Susan Ehrlich is the CEO of San Francisco General Hospital (SFGH). Despite the oncoming challenges, she reiterated that SFGH would remain true to its mission. “We want to make sure that the services we’re providing we’re doing with the highest quality of care, the safest care, but with the least amount of money,” she said.
Ultimately, Ehrlich expressed gratitude for San Francisco. “One thing that I feel really grateful about at this time is that we live in a city that is very devoted to taking care of its population and making sure that it takes care of the people, especially, who are the least well off,” she said. “That’s not true in every place in the United States.”